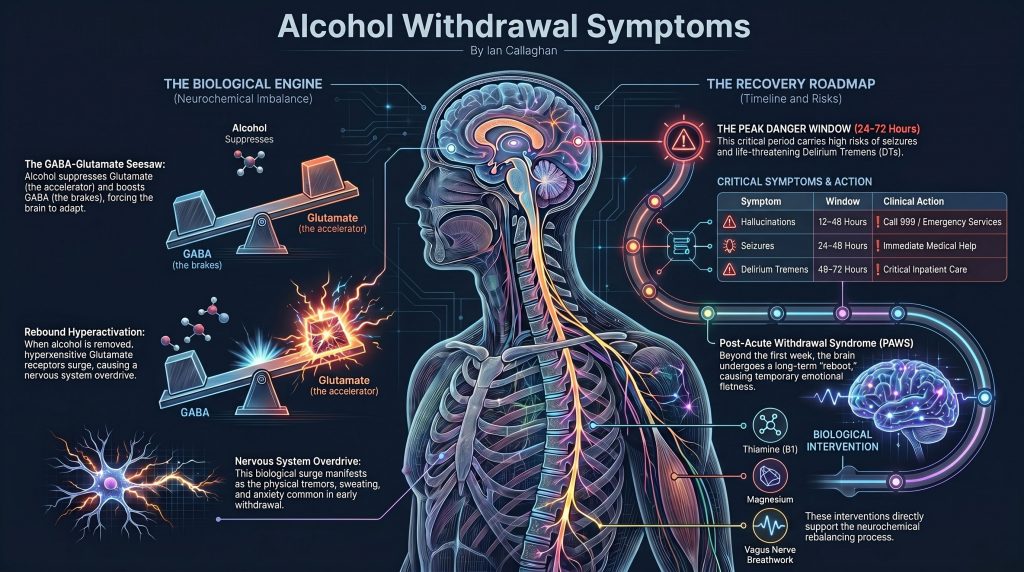
Alcohol withdrawal symptoms occur when the brain’s chemical balance is disrupted after stopping or significantly reducing alcohol. They typically begin 6 to 12 hours after the last drink and include anxiety, tremors, sweating, nausea, and insomnia. Symptoms peak between 24 and 72 hours. Severe symptoms — including seizures and delirium tremens — can be life-threatening and require immediate medical attention. Alcohol withdrawal happens because chronic drinking forces the brain to adapt its neurotransmitter systems. When alcohol is removed, those adaptations cause a rebound of neurological hyperactivity. This is a medical event, not a character failing.
Author: Ian Callaghan | Reiki Master | Sobriety and Nervous System Coach | Author of Under Load and Sober Beyond Limits | 45 years of lived experience with alcohol | Monmouthshire, UK
Introduction
You stopped drinking.
Maybe last night. Maybe three days ago. Maybe you’re planning to stop tonight, and you want to know what’s coming.
Either way, your body is doing something right now that nobody has properly explained to you. Not the NHS leaflet. Not the AA pamphlet. Not the well-meaning person who told you to drink more water and get an early night.
This is what’s actually happening — the mechanism, the timeline, the symptoms that are uncomfortable but normal, and the ones that mean you need medical help immediately.
No judgment. No agenda. Just the biology.
I am Ian Callaghan. I drank for 45 years. I know this territory from both sides — from the inside, and from the science I went looking for when I finally needed to understand what my body had been doing all that time.
If you want to understand how dangerous withdrawal can be before reading further, I have written a dedicated piece on exactly that: how dangerous are alcohol withdrawals when you stop drinking. This post covers the full neuroscience and mechanism underneath it.
What Are Alcohol Withdrawal Symptoms?
Alcohol withdrawal symptoms are the physical and psychological effects that occur when someone who has been drinking heavily stops or significantly reduces their alcohol intake.
They happen because alcohol is not just a drink. It is a central nervous system depressant that, over time, physically restructures the way your brain regulates itself. When you remove it, the brain doesn’t simply return to normal. It overshoots in the opposite direction.
The result is a nervous system in temporary overdrive — anxious, hyperactivated, and struggling to rebalance without the chemical it has been built around.
Why Does Alcohol Withdrawal Happen? The Brain Chemistry Explained
What Alcohol Does to Your Brain Over Time
Your brain runs on a careful balance between two primary neurotransmitters.
GABA — gamma-aminobutyric acid — is your brain’s braking system. It slows neural activity, reduces anxiety, and promotes calm and relaxation.
Glutamate is your brain’s accelerator. It drives alertness, energy, excitation, and cognitive arousal.
In a healthy brain, these two systems hold each other in check. The balance between them determines how activated or calm your nervous system runs at any given moment.
Alcohol hijacks this system. Every drink artificially boosts GABA and simultaneously suppresses glutamate. That is why alcohol feels the way it does — the brakes come on, the accelerator goes quiet, you relax, your inhibitions drop, and your anxiety reduces.
But your brain is not passive. It is constantly trying to maintain homeostasis — balance. And it adapts to the repeated chemical override.
Over weeks, months, and years of regular drinking, the brain compensates. It downregulates GABA receptors, reducing their sensitivity. It upregulates glutamate receptors, making them hypersensitive. It is literally rebuilding its architecture around the alcohol, fighting to keep functioning normally despite the repeated chemical suppression.
This is why tolerance develops. This is why you need more to feel the same effect. And this is why stopping creates a crisis.
For a deeper breakdown of the full neurochemical picture — dopamine, serotonin, endorphins, and the reward system — read: The Brain Chemistry of Addiction.
What Happens When You Stop Drinking Alcohol
When you stop drinking, the alcohol leaves your system. But the receptor changes your brain made do not reverse overnight.
You are now sitting with weakened brakes and a hypersensitive accelerator — with nothing suppressing the system.
Glutamate surges. GABA cannot contain it. The nervous system goes into rebound hyperactivation.
That is alcohol withdrawal. A predictable neurological event with a known mechanism, a measurable timeline, and a clear set of inputs that either help or harm the recovery process.
What Happens to Your Body When You Stop Drinking Alcohol: The Full Timeline
Severity varies significantly based on the length and volume of drinking, individual neurobiology, and overall health. This is the general clinical map.
Hours 6–12: The First Wave Begins
Within six to twelve hours of the last drink, the rebound begins.
Symptoms at this stage:
- Anxiety appearing without an obvious cause
- Hand tremors and shakiness
- Sweating — often disproportionate to temperature
- Headache
- Nausea, sometimes vomiting
- Heart rate elevated or irregular
- Insomnia despite exhaustion
- Irritability, restlessness, skin-crawling sensation
This is the initial glutamate surge. The nervous system is in early hyperexcitation. Uncomfortable, but not dangerous at this stage for most people.
Hours 12–48: Peak Intensity
This is the hardest window for most people withdrawing from alcohol.
Symptoms at this stage:
- Worsening anxiety, potentially severe
- Pronounced tremors
- Profuse sweating
- Elevated blood pressure and heart rate
- Complete inability to sleep
- Hypersensitivity to light and sound
- Severe emotional instability — fear, rage, grief without a clear trigger
- In 2–8% of cases: hallucinations — auditory, visual, or tactile
If you are hearing voices, seeing things, or feeling sensations on your skin that are not there, this is a medical emergency. Call emergency services.
Hours 24–72: The Danger Window
Withdrawal seizures occur in up to 15% of people going through significant alcohol withdrawal, typically between 12 and 48 hours after the last drink. They can happen with no preceding warning signs. They are major motor seizures — full body convulsions.
If a seizure occurs: call emergency services immediately. Do not wait.
Delirium tremens (DTs) — the most severe form of alcohol withdrawal — typically emerges between 48 and 72 hours, though it can appear up to seven days after stopping. It affects 3–5% of people withdrawing from alcohol.
Symptoms of delirium tremens include:
- Severe confusion and disorientation
- Agitation and aggression
- High fever
- Rapid, irregular heartbeat
- Profuse sweating
- Hallucinations
- Seizures
Without treatment, delirium tremens can be fatal. With prompt medical intervention, survival rates are high. This is why medical supervision during high-risk withdrawal is not optional.
You are at higher risk of severe withdrawal if:
- You have been drinking heavily daily for months or years
- You have experienced withdrawal before, particularly if it was severe
- You have previously had a withdrawal seizure
- You have liver disease, heart conditions, or other significant health conditions
- You are stopping abruptly after a very high daily consumption
If any of these apply, speak to a doctor before stopping. Read the full breakdown of risk factors here: How dangerous are alcohol withdrawals when you stop drinking?
Days 4–7: The Climb Down
For most people without severe complications, symptoms begin to ease after 72 hours. The acute glutamate surge starts to settle. GABA receptor sensitivity begins to recover.
Sleep remains disrupted. Anxiety continues at a lower level. Brain fog, physical fatigue, and emotional flatness are common. But the acute danger window has passed for most people.
For a detailed look at the biological recovery timeline from this point forward: physiology of alcohol recovery timeline.
Beyond Day 7: Post-Acute Withdrawal Syndrome (PAWS)
This is the part nobody tells you about. And the part that derails more recoveries than the acute phase ever does.
For many people — particularly those who drank heavily for years — a subtler, longer withdrawal phase follows the acute period—clinically referred to as post-acute withdrawal syndrome, or PAWS.
PAWS symptoms can include:
- Persistent sleep disruption — weeks or months of broken, unrefreshing sleep
- Mood instability — depression, anxiety, emotional blunting alternating unpredictably
- Cognitive fog — slow thinking, poor concentration, difficulty retaining information
- Anhedonia — the inability to feel pleasure or motivation from things that previously provided it
- Cravings arrive in waves, often triggered by stress, poor sleep, or emotional states
- Low energy and flat affect that feels indistinguishable from depression
The anhedonia piece catches most people completely off guard. If sobriety feels grey, flat, and pointless — that is not a sign that you were better off drinking. That is your dopamine system rebooting after years of chemical override. Read the full breakdown: anhedonia in early sobriety.
The gut-brain axis is also a key driver of PAWS that most withdrawal conversations completely ignore. Chronic alcohol use devastates the gut microbiome, which directly impacts neurotransmitter production, mood regulation, and the stress response. The nervous system cannot fully stabilise while the gut remains dysbiotic. This is not a side issue — it is central to why PAWS drags on—full explanation here: gut-brain axis and alcohol recovery.
GABA and glutamate function largely normalises within one to three months. Dopamine and serotonin systems take longer. Research suggests full neurochemical normalisation can take up to a year or more for long-term heavy drinkers.
This is not permanent damage in most cases. It is a healing process with a timeline.
Understanding that the flatness, the fog, and the low mood are mechanistic — that they are your brain rebuilding, not evidence that sobriety feels worse than drinking — changes everything about how you move through it.
What Helps During Alcohol Withdrawal: The Biology of Recovery
These are not wellness suggestions. These are inputs that directly support the neurochemical rebalancing process.
Hydration and Electrolytes
Sweating during withdrawal rapidly depletes sodium, potassium, and magnesium. Water alone does not replace them. Electrolyte-rich fluids, broth, and real food, which are tolerable, support the cellular environment the nervous system needs to repair.
For a clear guide on what to eat during early recovery: what to eat in early sobriety.
Magnesium
Magnesium is directly involved in GABA receptor function and nervous system regulation. It is aggressively depleted by chronic alcohol use. Supplementing during and after withdrawal — magnesium glycinate or citrate for absorption — directly supports the GABA recovery process.
B Vitamins — Particularly Thiamine (B1)
Alcohol depletes thiamine at an extreme rate. Thiamine deficiency during withdrawal can cause Wernicke’s encephalopathy — a serious neurological complication involving confusion, coordination problems, and vision changes. B complex supplementation in the early days of cessation is protective, not optional. If in any doubt, speak to a doctor about injectable thiamine.
Breathwork — The Vagus Nerve Mechanism
The glutamate surge drives sympathetic nervous system dominance — the fight-or-flight state running at full activation. Extended exhale breathing — where the exhale is longer than the inhale — directly activates the vagus nerve and shifts the autonomic nervous system toward parasympathetic dominance.
This is not relaxation advice. This is a direct mechanical intervention on the nervous system hyperactivation, driving withdrawal symptoms.
A simple starting point: inhale for four counts, exhale for six to eight. Five minutes. Notice what shifts.
The vagus nerve is the biological mechanism underneath this. For a full explanation of how it works and why it matters in recovery: vagus nerve and mental health. And specifically, how the vagal brake functions as your nervous system’s self-regulation switch.
Cold Water Exposure
Brief cold showers or cold water immersion create a controlled acute stress response that, when repeated, trains the nervous system back toward regulation. The initial shock, followed by the physiological adaptation, builds vagal tone — the nervous system’s capacity to self-regulate. Start with thirty seconds at the end of a normal shower and build from there.
Full protocol for using cold water to reclaim nervous system function in recovery: cold water reset — how to reclaim your nervous system naturally.
Sleep — Even Broken Sleep
The brain does the majority of its repair and neurotransmitter synthesis during sleep. Keep the environment dark, cool, and free of screens. Even lying still with eyes closed — without full sleep — allows the nervous system to recover partially.
Do not use alcohol to sleep. The sedation it creates is not restorative sleep. It actively prevents REM and deep sleep stages, during which neurological repair occurs.
Gentle Movement
Rhythmic movement — walking, slow bodyweight exercises — helps clear elevated cortisol and stress hormones and supports the production of endorphins and dopamine through natural pathways. Do not push through exhaustion. Move enough to shift the chemical state without depleting what little reserve you have.
When To Get Medical Help — No Ambiguity Here
Call 999 or go to A&E immediately if you experience:
- Seizures or convulsions of any kind
- Severe confusion or disorientation — not knowing where you are or what is happening
- Hallucinations — seeing, hearing, or feeling things that are not there
- High fever combined with agitation
- Extremely rapid or irregular heartbeat
- Loss of consciousness
Speak to a doctor before stopping drinking if:
- You have been drinking heavily daily for more than a few weeks
- You have withdrawn before, and it was severe or involved seizures
- Do you have any existing medical conditions, particularly heart or liver-related
- Are you on any medications that may interact with withdrawal
Do not attempt to manage high-risk withdrawal alone. Medical supervision and, where necessary, medication make this significantly safer. That is a clinical fact, not a judgment on your capacity to cope.
Full risk breakdown: How dangerous are alcohol withdrawals when you stop drinking?
How to Stop Drinking Alcohol: What Comes After the Acute Phase
Getting through withdrawal is the beginning, not the end.
The nervous system that was built around alcohol does not simply reset when the acute symptoms resolve. The reward circuitry, the stress response architecture, the gut-brain communication pathways — all of them were shaped by years of chemical intervention. All of them need deliberate rehabilitation.
The work that comes after acute withdrawal — rebuilding GABA naturally, restoring gut-brain axis function, recalibrating the stress response, rebuilding dopamine pathways through earned reward rather than chemical shortcut — is where most people either find solid ground or relapse back into the same loops.
If you are quitting cold turkey, read this first: Quitting Cold Turkey — The Risks, the Reality, and How to Do It as Safely as Possible.
If you survived the early days and are now navigating the harder, quieter stretch that follows: surviving the early days of quitting alcohol.
That is the work. And it is available to anyone willing to approach it with the right information.
FAQ: Alcohol Withdrawal Symptoms
How long do alcohol withdrawal symptoms last? Acute alcohol withdrawal symptoms typically begin within 6 to 12 hours of the last drink, peak between 24 and 72 hours, and resolve for most people within 5 to 7 days. However, post-acute withdrawal syndrome (PAWS) can persist for weeks to months, with symptoms including sleep disruption, mood instability, cognitive fog, and cravings.
What are the first signs of alcohol withdrawal? The first signs of alcohol withdrawal typically appear 6 to 12 hours after the last drink and include anxiety, hand tremors, sweating, headache, nausea, elevated heart rate, and insomnia. These early symptoms reflect the initial GABA-glutamate rebound in the brain.
Can alcohol withdrawal kill you? Yes. Severe alcohol withdrawal can be fatal without medical intervention. Delirium tremens — which affects 3 to 5% of people withdrawing from alcohol — can cause fatal cardiovascular and neurological complications if untreated. Withdrawal seizures, which occur in up to 15% of significant withdrawal cases, also carry risk. Anyone at high risk of severe withdrawal should seek medical supervision before stopping.
What happens to your body when you stop drinking alcohol? When you stop drinking alcohol, your brain enters a rebound state. The GABA system — suppressed by chronic alcohol use — becomes underactive. The glutamate system — also chronically suppressed — rebounds into hyperactivity. This neurological imbalance produces the physical and psychological symptoms of withdrawal. Over days to weeks, the brain begins to rebalance its neurotransmitter systems and restore natural regulation.
What is the difference between a hangover and alcohol withdrawal? A hangover is the acute aftermath of a single drinking session — dehydration, acetaldehyde toxicity, disrupted sleep, and a mild GABA-glutamate rebound. Alcohol withdrawal is a distinct medical condition that occurs in people with physical dependence on alcohol, where the brain has structurally adapted to alcohol’s presence and cannot function normally without it. Withdrawal symptoms are more severe, more prolonged, and potentially life-threatening in a way that a hangover is not.
What is alcohol cessation syndrome? Alcohol cessation syndrome is another term for alcohol withdrawal syndrome — the collection of physical and neurological symptoms that occur when a person who is physically dependent on alcohol stops or reduces their intake. It ranges from mild anxiety and tremors to potentially fatal complications, including seizures and delirium tremens.
How do you stop drinking alcohol every night safely? If you drink heavily every night and want to stop, the safest approach is to speak to a doctor first. For mild dependence, a gradual reduction may be appropriate. For moderate to severe dependence, medically supervised detox reduces the risk of serious complications. After the acute phase, the focus shifts to nervous system rehabilitation — rebuilding natural regulation through nutrition, sleep, breathwork, movement, and gut-brain axis recovery.
Why do I feel anxious and shaky after stopping drinking? Anxiety and shakiness after stopping drinking are direct symptoms of the GABA-glutamate rebound. Alcohol artificially boosted GABA (the calming neurotransmitter) and suppressed glutamate (the excitatory neurotransmitter) during drinking. When alcohol is removed, glutamate surges back while GABA remains underactive, creating a state of neurological hyperexcitation that manifests as anxiety, tremors, and physical agitation.
Does alcohol withdrawal get worse each time? Yes, in many cases. This is known as the kindling effect — each episode of withdrawal can sensitise the brain’s excitatory systems, making subsequent withdrawals more severe. This is one of the key reasons why medically supervised management of withdrawal is important, particularly for anyone who has withdrawn multiple times before.
What is post-acute withdrawal syndrome (PAWS)? Post-acute withdrawal syndrome (PAWS) is the prolonged phase of withdrawal that follows the acute stage. It can last weeks to months and includes symptoms such as persistent insomnia, mood instability, cognitive fog, anhedonia, and intermittent cravings. PAWS is driven by the slow rebalancing of neurotransmitter systems — particularly dopamine and serotonin — and the ongoing recovery of the gut-brain axis after years of alcohol-related damage.
The Bottom Line on Alcohol Withdrawal Symptoms
Alcohol withdrawal is your nervous system reclaiming itself.
It is painful. In some cases, it is dangerous. But what is happening underneath — the GABA receptor recovery, the glutamate settling, the slow return of natural dopamine and serotonin regulation — is your brain learning to function again without a chemical it was built around.
The acute phase ends. The fog begins to lift. The flatness gives way — not all at once, but incrementally, measurably, if you give the biology the right conditions to complete the work.
Most people who relapse do so not during acute withdrawal but during the weeks that follow — when the brain’s reward system is still offline, when sleep is still broken, when the reasons they drank are still present, but the chemical relief is gone.
That gap is where the real work lives. And it has a framework.
If you are in the early days and want to understand the full neurological picture of what comes after withdrawal — and what the rebuild actually looks like:
If you want to talk through where you are right now:
Join the community where this conversation continues every week:
This article is for informational purposes only and does not constitute medical advice. If you are experiencing severe alcohol withdrawal symptoms, contact emergency services or your doctor immediately. Alcohol withdrawal can be life-threatening. You do not have to manage it alone.
Ian Callaghan is a sobriety coach, Reiki Master, and author based in Monmouthshire, Wales. He writes from 45 years of lived experience with alcohol and a decade of research into the neuroscience of addiction and recovery.