Heart Rate Variability: The One Number That Tells You Everything About Why You Feel the Way You Do in Midlife
By Ian Callaghan | iancallaghan.co.uk |Heart Rate Variability Midlife
Heart rate variability midlife. You wake up tired. Not the kind of tired that a good night’s sleep fixes. The kind that sits behind your eyes and follows you into the afternoon. Your focus is soft. Your mood is lower than it should be. You’re doing everything vaguely right. You’re not drinking that much, you’re not eating terribly, you’re getting to bed at a reasonable hour, and yet something in the machinery feels off.
You’ve probably blamed it on stress. On age. On the relentlessness of midlife.
Most people do.
But there is a number your body is generating every single morning that tells a different story. A number that most people have never heard of, that their GP has almost certainly never mentioned, and that quietly predicts cardiovascular health, cognitive function, metabolic resilience, emotional regulation, and how fast you are ageing at a biological level.
That number is your Heart Rate Variability. And once you understand what it is, what it measures, and what is suppressing it in your specific life, you cannot unknow it.
This is not a biohacker post. This is not for elite athletes or tech bros with six wearables. This is for the woman in her late forties who is tired of being told she needs to manage her stress better. This is for anyone in midlife who suspects that the way they feel is not inevitable but has not yet found a clear enough explanation of the mechanism to do anything about it.
Here is that explanation.
What Is Heart Rate Variability and Why Does It Matter?
Heart Rate Variability, or HRV, is the variation in time between consecutive heartbeats, measured in milliseconds.
A heart beating at 60 beats per minute does not beat with mechanical precision, beating once every 1,000 milliseconds. The gaps between beats vary. Sometimes 980ms. Sometimes 1,040ms. Sometimes 1,010ms. This variation is not a malfunction. It is a feature. And that variation is the signal.
More variability between heartbeats means your autonomic nervous system is flexible, adaptive, and responsive. It means the parasympathetic branch. Your rest, digest, recover, and repair system. It is functioning well. It means your body can shift between states efficiently. High HRV is broadly associated with resilience across physiological, psychological, and metabolic domains.
Less variability means your nervous system is under strain. The gaps between beats become more uniform, more rigid. Your body is locked in a state of low-grade alert, running on its stress architecture rather than its recovery architecture. Low HRV is independently associated with elevated cardiovascular risk, insulin resistance, faster cognitive decline, anxiety, depression, and burnout.
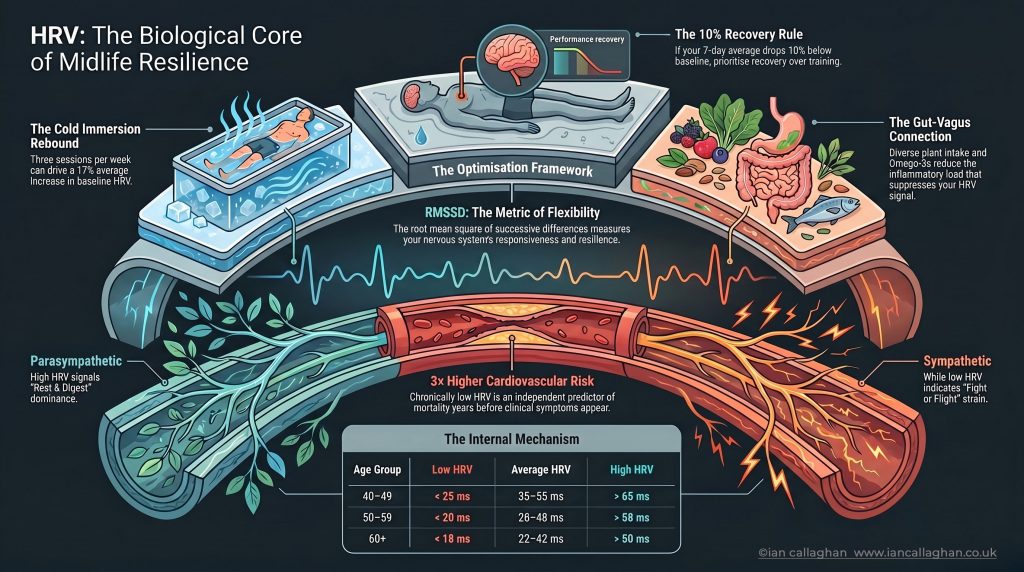
The key measurement is called RMSSD (root mean square of successive differences). This is what your wearable reports when it displays an HRV number. It reflects parasympathetic nervous system activity. The higher it is, the more your body is in recovery mode. The lower it is, the more it is in damage limitation mode.
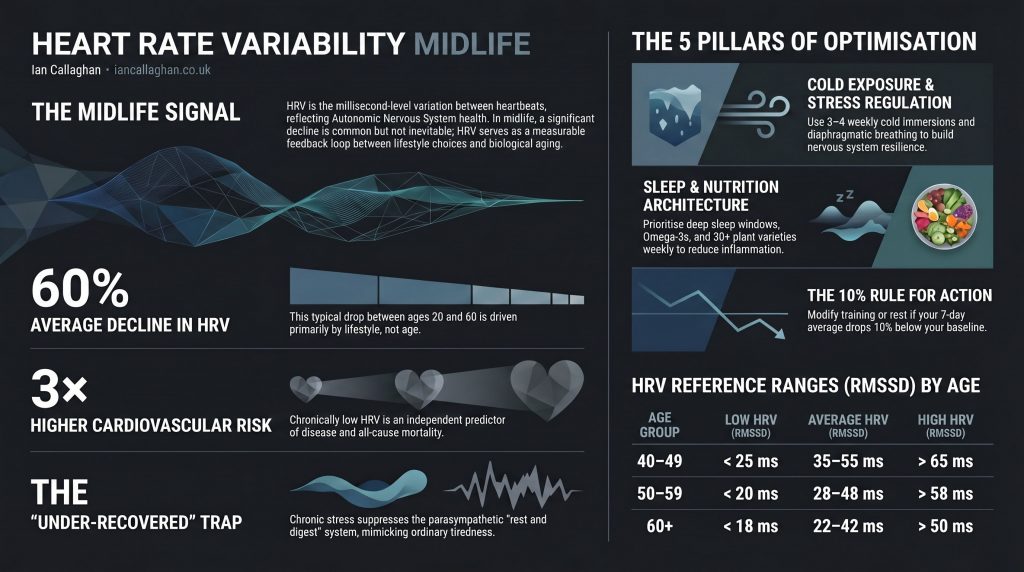
This is why HRV matters specifically in midlife. The average HRV declines by roughly 60% between the ages of 20 and 60. But this is the part the fitness industry consistently fails to communicate clearly: that decline is not inevitable. It is driven overwhelmingly by lifestyle inputs. Aerobically fit 50-year-olds routinely show HRV values that match sedentary 30-year-olds. The gap is in inputs, not age.
The choices being made right now in your 40s and 50s are not just affecting how you feel this week. The choices being made now are setting the trajectory of your autonomic nervous system for the next three decades.
The Autonomic Nervous System: Understanding the Engine
To understand HRV, you need to understand the system it is measuring: your autonomic nervous system. This is the part of your nervous system that runs without your conscious input. It controls heart rate, digestion, immune function, respiratory rate, and the hormone cascade that governs how your body responds to both threat and safety.
It has two primary branches.
The sympathetic nervous system is your fight-or-flight system. It is activated by stress, threat, exertion, or perceived danger. It releases adrenaline and cortisol. It speeds the heart rate, narrows the variability between beats, and prepares the body for action. It is essential and life-saving in acute situations. It is destructive when it runs chronically.
The parasympathetic nervous system is your rest-and-digest system. It is activated during calm, during sleep, and during genuine recovery. It is mediated primarily by the vagus nerve. The longest cranial nerve in the body runs from the brainstem through the heart, lungs, and gut. When parasympathetic tone is high, heart rate slows, beat-to-beat variability increases, digestion functions well, inflammation decreases, and the body performs the repair work it needs.
HRV is, in functional terms, a proxy for parasympathetic nervous system health. A high HRV reading tells you that your vagus nerve is doing its job. A low HRV reading tells you something is suppressing it.
Most people in midlife are living with chronically suppressed parasympathetic activity and have no framework for understanding why they feel the way they feel. They are not burned out in the dramatic clinical sense. They are chronically under-recovered. And the difference between those two diagnoses matters enormously for how you intervene.
What HRV Is Actually Telling You: The Clinical Picture
Low HRV is not just a fitness metric. The research connecting HRV to broader health outcomes is substantial, consistent, and largely ignored outside specialist clinical settings.
Cardiovascular health. HRV is an independent predictor of cardiovascular disease and all-cause mortality. Chronically low HRV appears in the data years before clinical symptoms of cardiovascular disease emerge. People with consistently low HRV face roughly triple the cardiovascular event risk of age-matched peers with healthy HRV.
Metabolic function. HRV is strongly correlated with insulin resistance, metabolic syndrome, and elevated inflammatory markers, including C-reactive protein and interleukin-6. If you are struggling with unexplained weight gain, persistent belly fat that does not respond to diet changes, or energy crashes after meals, your HRV data may be part of the picture your GP is not seeing.
Cognitive function. Higher HRV is associated with better working memory and executive function. Low HRV predicts faster cognitive decline with age. The connection is not incidental. The vagus nerve, which drives parasympathetic tone, also innervates the prefrontal cortex, which governs focus, decision-making, and emotional regulation.
Mental health. Low vagal tone is a documented feature of clinical anxiety, depression, and burnout. The vagus nerve directly feeds into mood regulation circuits. This is not a metaphor about stress management. It is physiology. Your emotional landscape is partly a readout of your autonomic nervous system state.
Physical recovery. Post-exercise HRV suppression lasting more than 48 hours signals overreaching. The body is breaking down rather than adapting. If you are training and not recovering, your HRV will show it before your subjective experience does.
Sleep quality. HRV rises through the night, peaking before natural waking during deep slow-wave sleep. Any disruption, a late meal, alcohol, noise, or temperature. Each one blunts this rise. Your morning HRV reading is effectively a report card on how well your body recovered overnight. When it is consistently low, something in the overnight environment or the preceding day’s inputs is working against you.
The Midlife Trap: Why Your Nervous System Is Under Silent Siege
Here is what happens specifically in midlife that most health content fails to address clearly.
Chronic psychological stress. The kind that accumulates over years of responsibility, invisible labour, career pressure, relationship complexity, and the relentless demands of midlife. All of it keeps cortisol elevated well beyond its normal morning peak. In a healthy cortisol pattern, levels spike at waking and decline steadily through the day. In a chronic stress pattern, cortisol remains elevated throughout the day and fails to drop adequately at night.
This chronically elevated cortisol directly and measurably suppresses parasympathetic activity. It narrows HRV. Over months and years, this creates what looks, from the outside, like ordinary tiredness, and what feels, from the inside, like a slow loss of the version of yourself you used to be.
For women moving through perimenopause and menopause, this picture is compounded by hormonal changes that independently affect HRV. Oestrogen has a protective effect on autonomic function. As oestrogen declines, the nervous system becomes more vulnerable to sympathetic dominance. This is one of the mechanisms behind the sleep disruption, anxiety, brain fog, and emotional volatility that many women in their late 40s and 50s experience, and it is under-discussed in clinical settings and almost absent from mainstream wellness content.
The connection between perimenopause and HRV is a blue ocean of understanding that most healthcare systems have yet to reach. Women are told their symptoms are hormonal, which is partly true, but the nervous system story, and crucially, what you can do about it. That part is rarely part of the conversation.
The good news, and it is really good news, is that HRV responds rapidly and measurably to specific lifestyle inputs. The decline is addressable. The research is consistent. And several of the most powerful interventions cost nothing.
What Is Destroying Your HRV: The Suppressors
Before looking at what raises HRV, it is worth being clear about what tanks it. This section will be uncomfortable for some people. It is meant to be informative, not moralistic.
Alcohol
Alcohol is the most potent dietary suppressor of HRV that has been studied. A single drink the evening before measurably reduces morning HRV by 10-15%. Two drinks produce a 20-25% reduction. The data here is remarkably consistent across multiple studies and wearable datasets.
The mechanism is straightforward. Alcohol disrupts the parasympathetic rebound that should occur during deep sleep. It fragments sleep architecture, suppresses slow-wave sleep, increases overnight cortisol, and elevates resting heart rate. All of this narrows beat-to-beat variability and shows up clearly in your morning reading.
This is not a moral position on alcohol. It is a measurement. Your wearable does not have opinions. It just reports what happened to your autonomic nervous system overnight.
The HRV data on alcohol removal are equally consistent. Removing alcohol produces an average 14% improvement in HRV over four to six weeks. For a woman in her late 40s already navigating perimenopause-related HRV decline and sleep disruption, that is not a small number. That is a meaningful shift in nervous system function that will show in how she thinks, feels, recovers, and ages.
Ultra-Processed Food
Ultra-processed foods disrupt the gut microbiome and increase intestinal permeability. What is commonly called “leaky gut” elevates circulating lipopolysaccharide, a bacterial endotoxin. This LPS triggers systemic inflammation. That inflammation suppresses vagal tone. Suppressed vagal tone lowers HRV.
The gut-vagus connection is underappreciated even within functional health communities. 80% of vagal fibres are afferent. They travel from gut to brain, not the reverse. Your gut is not passively receiving instructions from your nervous system. It is actively sending signals upward continuously, and the quality of those signals is determined by what you feed your microbiome.
A diet high in ultra-processed food sends inflammatory signals up the vagus nerve to the brain, suppressing parasympathetic activity and reducing HRV. A diet rich in diverse whole foods, fermented foods, and anti-inflammatory fats sends the opposite signal.
High-Glycaemic Eating Patterns
Large blood sugar spikes trigger the release of adrenaline and cortisol as the body scrambles to manage glucose levels. This pattern repeats multiple times throughout the day, sustaining sympathetic nervous system dominance and chronically suppressing HRV. It is not dramatic. It does not feel like stress. It just keeps the nervous system running slightly too hot, day after day, year after year.
Poor Sleep and Circadian Disruption
One poor night reduces next-day HRV by 8-12%. Two consecutive poor nights can suppress HRV for three to four days, even with normal sleep afterwards. Irregular sleep and wake times, blue light exposure after 9 pm, late-night eating, and chronic circadian disruption all compound this effect. The overnight HRV curve relies on consistency. Disrupt the conditions,s and you disrupt the recovery.
What Raises HRV: The Protocol That Works
The research here is consistent, and the interventions are accessible. You do not need a £400 supplement stack or a clinic appointment.
Cold Water Immersion
Cold water immersion is the fastest-acting HRV intervention available and the most underutilised outside elite sport. The mechanism works in three phases.
In the first 60 seconds, sympathetic shock occurs. Heart rate spikes, breathing shortens, and cortisol briefly rises. This is the stimulus, and this is the point. That acute stress is what drives the adaptation.
Between 60 and 180 seconds, if you control your breathing and do not fight the cold, the body shifts decisively toward parasympathetic dominance. Norepinephrine surges by up to 300%. Vagal tone increases sharply. This parasympathetic rebound is the mechanism behind HRV gains from cold exposure.
Over days and weeks of repeated exposure, chronic cold immersion recalibrates the autonomic set point. Resting parasympathetic tone increases. Basal heart rate decreases. HRV rises measurably.
The research shows an average RMSSD improvement of 17% after four weeks of cold water immersion, three times per week, at 10 to 15 degrees Celsius for three to five minutes. Resting morning cortisol also drops by approximately 14% after six weeks of regular cold exposure, and lower baseline cortisol directly enables higher baseline HRV.
I swim in the River Usk year-round. In October, the water temperature drops to 10-12 degrees Celsius. I have been doing this for over 50 years. Long before it had a name. I understand it now, through the HRV data, in a way I could not have articulated before. The mechanism explains the experience. Every session is a deliberate recalibration of the autonomic nervous system.
The entry point is not a cold river. It is ending your shower with 30 seconds of cold water. That is week one. The body adapts faster than most people expect.
Anti-Inflammatory Nutrition
Omega-3 fatty acids, from oily fish, specifically EPA and DHA, directly increase cardiac parasympathetic modulation. This is one of the most replicated nutrition-HRV findings in the literature. Two to three portions of oily fish per week is the evidence-based recommendation.
Diversity of plant foods is the single most powerful microbiome intervention available. Thirty different plant varieties per week, including vegetables, fruits, legumes, whole grains, nuts, seeds, and herbs. That diversity drives microbiome diversity, reduces inflammatory signalling, and measurably improves vagal tone over four to six weeks.
Fermented foods (kefir, kimchi, sauerkraut, live yoghurt) deliver live cultures that modulate microbiome composition and reduce the inflammatory markers most directly associated with low HRV.
Magnesium is rate-limiting for parasympathetic neurotransmission. Up to 60% of adults are deficient. Dark leafy greens, pumpkin seeds, and black beans are the food-first approach before considering supplementation.
Sleep Architecture
HRV recovery does not happen during the day. It happens at night, in deep slow-wave sleep, via the parasympathetic nervous system. Protecting the conditions for deep sleep is not optional if you are serious about moving your HRV.
A fixed wake time anchors the circadian rhythm more powerfully than any other single sleep intervention. A room temperature of around 17 degrees Celsius is optimal for deep sleep. No screens for 60 minutes before bed protects melatonin production. No alcohol within three hours of sleep protects sleep architecture. An evening walk helps lower cortisol before the body needs to shift into parasympathetic dominance overnight.
Stress Regulation and Vagal Tone
Breathwork, specifically slow diaphragmatic breathing at around six breaths per minute, directly stimulates the vagus nerve and produces measurable acute increases in HRV. Zone 2 cardiovascular exercise, morning light exposure within 30 minutes of waking, and meditation all build parasympathetic capacity, which cold exposure then amplifies.
These are not lifestyle suggestions. They are inputs to a system that produces measurable outputs. Your wearable will show you the data if you track consistently.
How to Read Your HRV Numbers
The reference ranges for RMSSD by age give useful context, but your personal trend over 14 or more days matters far more than any population benchmark.
For those aged 40 to 49, the average RMSSD ranges from 35 to 55 milliseconds. Below 25 is clinically low. Above 65 is strong. For the 50-59 age group, the average is 28-48 milliseconds. Below 20 is low. Above 58 is strong. For those over 60, the average is 22-42 milliseconds.
The 10% rule is your practical daily guide. If your 7-day HRV average drops 10% or more below your 30-day personal baseline, your body is signalling stress, illness, or overtraining. This is your cue to reduce load and prioritise recovery, not push harder.
Never act on a single data point. Act on trends. Consistency of measurement matters more than the absolute number. Measure at the same time each morning, before coffee, in the same posture.
How to Measure HRV
Consumer wearables (Oura Ring, WHOOP, Apple Watch) provide automated overnight measurement. Convenient and consistent. Sufficient for lifestyle feedback and trend tracking. Accuracy varies by device and skin tone.
For greater precision, a Polar H10 chest strap, used with the free HRV4Training app, provides gold-standard accuracy for a one-minute morning measurement. This is the approach used in most of the research. It removes the confounds of sleep movement that can affect optical sensors.
The protocol is simple: at the same time each morning, before coffee, lying or sitting in a consistent posture. One minute. Every day. Your data becomes meaningful over 14 days and increasingly useful over 30.
Your 30-Day Starting Point
Week one: establish your baseline. Get a wearable or download HRV4Training. Measure every morning. Log your sleep, your alcohol intake, your stress levels, and your food. Do not change anything yet. Just observe. The data at the end of week one will tell you more than any article can.
Week two: add your first interventions. End every shower with 30 seconds of cold water. Set a fixed wake time and stick to it regardless of when you went to bed. Add 10 minutes of outdoor morning light within 30 minutes of waking. If you drink alcohol, remove it for the week and track the HRV response. The data you generate in week two is one of the most instructive things you can do for your own health literacy.
Week three: move to cold bath or open water immersion three to four times per week. Actively track plant variety in your food. Add an omega-3 source daily. Add one fermented food daily. Watch your 7-day average.
Week four: compare your 7-day average to week one. Identify which interventions had the greatest impact on your number. That is your personalised protocol. Not mine. Yours.
The Honest Position on All of This
I am a coach and a chef. I have spent 40 years paying attention to food. I have been going into the River Usk for over 50 years. Long before it had a name. Long before it had a hashtag. Long before anyone called it cold water therapy or gave it a protocol. I have spent 15 years working with people in midlife, men and women both, navigating exactly the territory this post describes.
I am not a clinician. The research I have referenced throughout this post is real and accessible. I am not asking you to take my word for anything. I am asking you to take your own data seriously.
What I can say with complete confidence is this. The way most people in midlife feel is not inevitable. It is not just getting older. It is an input problem. Specific, addressable, and measurable. HRV is the tool that closes the feedback loop between what you are doing and how it affects your body.
The number your heart generates every morning is trying to tell you something. Most people never learn to listen to it.
That is the part that frustrates me most. Not because the information is inaccessible. It is not. But because nobody translated it for the people who need it most, in a language that they understand.
That is what this post is for.
Frequently Asked Questions About Heart Rate Variability
What is a good HRV score for a woman in her 40s or 50s?
There is no single good number because HRV is highly individual. As a general reference, women aged 40 to 49 typically have an RMSSD between 35 and 55 milliseconds on average. For 50 to 59, the average range is 28 to 48 milliseconds. What matters far more than hitting a population benchmark is your personal trend. A consistent upward trend in your own baseline over 14 to 30 days is the signal to pay attention to, not whether you match someone else’s number.
Does alcohol really affect HRV that much?
Yes, and the data is among the most consistent in this field. A single drink the evening before measurably suppresses morning HRV by 10-15%. Two drinks push that to 20-25%. The mechanism is straightforward: alcohol disrupts the parasympathetic rebound that occurs during deep sleep, fragments sleep architecture, and elevates overnight cortisol. Your wearable will show this the morning after a drink, even if you feel fine. It does not have opinions. It just reports what happened.
Can you improve HRV after 50?
Yes. This is one of the most important things the research shows clearly. The decline in HRV between your 20s and 60s is driven primarily by lifestyle inputs, not by age itself. Aerobically fit 50-year-olds routinely show HRV values that match sedentary 30-year-olds. Alcohol removal alone produces an average 14% HRV improvement over four to six weeks. Cold water immersion three times per week yields an average improvement of 17% over four weeks. The decline is not a sentence. It is a feedback loop you can change.
Does perimenopause affect HRV?
Yes, significantly and in ways that are rarely discussed in clinical settings. Oestrogen has a protective effect on the autonomic nervous system function. As oestrogen declines during perimenopause, the nervous system becomes more vulnerable to sympathetic dominance. This is part of the physiological mechanism behind the sleep disruption, anxiety, brain fog, and mood volatility that many women in their late 40s and 50s experience. It also means that lifestyle interventions that raise HRV, specifically cold exposure, anti-inflammatory nutrition, alcohol removal, and sleep consistency, are particularly valuable during this transition.
What is the best device to track HRV?
For everyday trend tracking, the Oura Ring, WHOOP, and Apple Watch all provide usable HRV data. None is clinical-grade, but all are sufficiently consistent for lifestyle feedback. For greater precision, the Polar H10 chest strap, used with the free HRV4Training app, provides gold-standard accuracy and is the basis for most peer-reviewed research. Whichever device you choose, consistency matters more than the device itself. Measure at the same time every morning, in the same posture, before coffee.
How quickly can you improve your HRV?
Faster than most people expect. Removing alcohol for a week will show measurable improvement in your 7-day average within days for most people. A single cold water immersion session produces an acute HRV boost in the hours following exposure. Sustained improvement in your 30-day baseline takes four to six weeks of consistent intervention. The interventions are not slow. Most people never start them because nobody explained the mechanism clearly enough to make it worth the effort.
Is low HRV dangerous?
Chronically low HRV is an independent predictor of cardiovascular disease, appearing in the data years before clinical symptoms emerge. It is also strongly correlated with insulin resistance, faster cognitive decline, clinical anxiety, and burnout. This does not mean a single low reading is cause for alarm. One poor night of sleep will drop your HRV. What matters is persistent, chronic suppression over weeks and months. If your 7-day average has been sitting 10% or more below your 30-day baseline for an extended period, that is a signal worth taking seriously and worth discussing with your GP.
What is the vagus nerve, and why does it matter for HRV?
The vagus nerve is the longest cranial nerve in the body, running from the brainstem through the heart, lungs, and gut. It is the primary mediator of parasympathetic nervous system activity, the branch of the autonomic nervous system responsible for rest, digestion, recovery, and repair. When vagal tone is high, HRV is high. When something suppresses vagal tone, including alcohol, ultra-processed food, chronic stress, and poor sleep, HRV drops. Practices that directly stimulate the vagus nerve, including cold water immersion, slow diaphragmatic breathing, and certain forms of meditation, raise HRV measurably. The vagus nerve is the hardware. HRV is the readout.
About Ian Callaghan
Ian Callaghan is a British Army veteran, qualified chef, NLP Master Practitioner, Reiki Master, and multi-disciplinary coach based in Monmouthshire, Wales. He has been swimming in the River Usk year-round for over 50 years, long before cold water immersion had a name or a hashtag. He works with midlife adults on the Total Systems Reset framework: food, sleep, movement, and mind, not as lifestyle aspirations but as engineering problems with measurable solutions.
His books, coaching programmes, and deep-dive resources are available at iancallaghan.co.uk. He runs the Sober Beyond Limits community on Facebook and the Ian Callaghan Midlife Reset community on Skool.
© Ian Callaghan | iancallaghan.co.uk

Under Load by Ian Callaghan | The Mechanical Guide to Addiction Recovery
You already know what you’re doing. You’ve known for years.

The 30-Day Reset: Reclaim Your Vitality, Rewire Your Mind, and Reboot Your Body (Digital Ebook)
The 30 Day Reset is not a diet. It is a complete biological overhaul for anyone who is wired, tired, and done with feeling like shite. The 30-Day Reset is a 160+ page military-grade systems reboot for the over-35s. Four pillars. Eat, sleep, move, mind. One month to strip out the industrial poison, reset your dopamine pathways, silence Bob, and rebuild the machine that’s been running on the wrong fuel for decades. Not a diet. Not a programme. A complete…